Overview
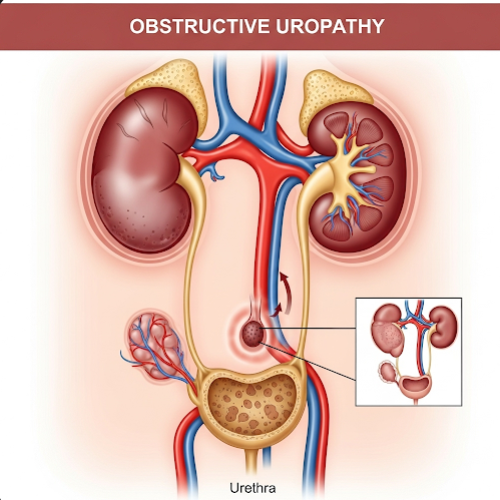
Obstructive uropathy is a condition where the normal flow of urine is blocked—either partially or completely—at any point in the urinary tract. This obstruction causes urine to back up into the kidneys, ureters, or bladder, which can lead to pain, infection, kidney damage, and even kidney failure if not treated promptly. Obstructive uropathy can be acute or chronic, unilateral or bilateral, and may affect people of any age, including infants and the elderly. The cause may be mechanical (like a kidney stone) or functional (such as an enlarged prostate or neurogenic bladder).
What is Obstructive Uropathy?
Obstructive uropathy refers to any blockage that prevents urine from exiting the kidneys, leading to hydronephrosis (swelling of the kidney) and other downstream complications. Obstruction can occur at different levels:
- Upper tract: kidneys or ureters
- Lower tract: bladder, prostate, or urethra
The obstruction increases pressure in the urinary system, impairing the kidneys’ ability to filter waste and regulate fluid and electrolytes.
Symptoms
Symptoms of obstructive uropathy vary based on the location, duration, and severity of the blockage.
Acute obstruction symptoms:
- Sudden severe flank or abdominal pain
- Decreased or absent urine output
- Nausea and vomiting
- Fever and chills (if infection is present)
- Hematuria (blood in urine)
Chronic obstruction symptoms:
- Frequent urinary tract infections (UTIs)
- Increased urinary frequency or urgency
- Weak urine stream or dribbling
- Back or flank pain
- Fatigue or malaise
- Hypertension
- Swelling in legs (in late stages)
Some patients, especially those with partial obstruction, may have no obvious symptoms until significant kidney damage has occurred.
Causes
Obstructive uropathy can be caused by a variety of anatomical or functional issues, including:
Upper urinary tract causes:
- Kidney stones (most common)
- Ureteral stricture or scarring
- Tumors of the kidney, ureter, or nearby organs
- Retroperitoneal fibrosis
- Congenital defects (e.g., ureteropelvic junction obstruction in children)
Lower urinary tract causes:
- Benign prostatic hyperplasia (BPH) in men
- Prostate cancer
- Bladder stones or tumors
- Neurogenic bladder (nerve damage affects bladder function)
- Urethral stricture
- Pelvic organ prolapse in women
Bilateral obstruction is particularly dangerous, as it affects both kidneys and can rapidly cause renal failure.
Risk Factors
Individuals are more likely to develop obstructive uropathy if they have:
- History of kidney stones or urinary tract infections
- Prostate enlargement or prostate cancer
- Pelvic or abdominal cancer
- Recent abdominal or urologic surgery
- Diabetes or neurological conditions affecting bladder control
- Congenital urinary tract anomalies
- Radiation therapy to the pelvic area
Complications
If untreated, obstructive uropathy can lead to:
- Hydronephrosis
- Kidney infection (pyelonephritis)
- Chronic kidney disease (CKD) or kidney failure
- Electrolyte imbalance
- Hypertension
- Sepsis, in cases of infected obstruction
- Bladder damage or incontinence
Early diagnosis and intervention are essential to prevent irreversible damage to the urinary system.
Prevention
While not all causes are preventable, you can reduce your risk of obstructive uropathy by:
- Staying hydrated to prevent kidney stones
- Managing BPH or prostate health through regular checkups
- Seeking prompt treatment for UTIs
- Avoiding prolonged use of bladder-irritating medications
- Monitoring and managing diabetes or neurological disorders
- Routine screenings for people with cancer or pelvic diseases
In children, prenatal ultrasounds may detect congenital urinary obstructions early.
Treatment Options in Korea
South Korea offers advanced diagnostic and treatment options for obstructive uropathy through leading urology, nephrology, and radiology departments.
1. Diagnosis
- Urinalysis and blood tests: Check kidney function and signs of infection
- Ultrasound: Non-invasive imaging to detect hydronephrosis
- CT scan or MRI: Detailed view of obstruction
- Voiding cystourethrogram (VCUG): Assesses bladder and urethral function
- Renal scintigraphy (DTPA or MAG3 scan): Evaluates kidney drainage
- Cystoscopy: Visual examination of the bladder and urethra
2. Medical Treatment
- Antibiotics for infection
- Alpha-blockers for BPH
- Pain relief and anti-inflammatory medications
- Temporary catheterization or stent placement to relieve obstruction
- Management of underlying conditions (e.g., diabetes, tumors)
3. Surgical Treatment
Depending on the cause, surgery may be required to relieve the blockage:
- Ureteral stent or nephrostomy tube for urgent decompression
- Ureteral dilation or laser treatment for strictures
- TURP (transurethral resection of the prostate) for BPH
- Stone removal (ureteroscopy, lithotripsy, or percutaneous surgery)
- Bladder or prostate tumor removal
- Corrective surgery for congenital defects in children
4. Top Hospitals and Urology Centers in Korea
- Asan Medical Center – Department of Urology
- Samsung Medical Center – Kidney and Urological Center
- Seoul National University Hospital – Urology and Nephrology
- Severance Hospital (Yonsei University) – Urology & Robotic Surgery
- CHA Bundang Medical Center – Women’s Urology and Pediatric Urology
These centers provide: - Minimally invasive surgery and robotic options
- Multilingual support for international patients
- Integrated care teams (urologists, nephrologists, radiologists)